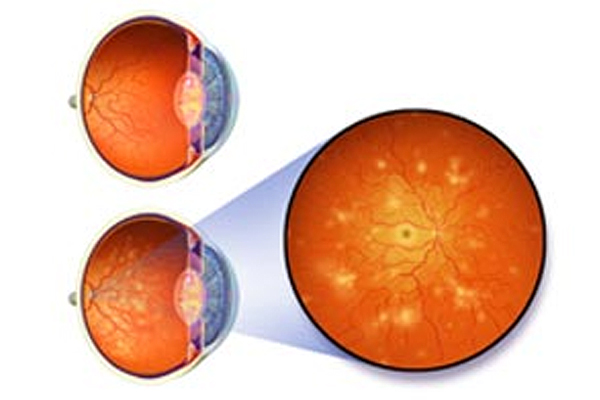
Diabetic retinopathy is a complication of diabetes that affects the eyes of people suffering from type 1 & type 2 diabetes. If you’ve had diabetes for long, you have greater chances of developing diabetic retinopathy. In the initial stages, it may only cause mild vision problems but can develop into complete blindness.
Protect your vision by keeping your sugar level in control and regularly going for eye check-ups. Screening for diabetic retinopathy should be done at the time of diagnosis in the case of type 2 diabetes and at 5 years in type 1 diabetes. Controlling blood sugar and blood pressure can slow or halt the progress of this disease and appropriate treatment can.
There are hardly any symptoms visible in the early stages of diabetic retinopathy. Eye examinations are the only way to keep diabetic retinopathy at bay. As the condition worsens, the following symptoms may be experienced:
Non-proliferative diabetic retinopathy (NPDR), where blood vessels in the retina deteriorate, either becoming blocked or deformed. Fluids, fats and proteins leak out of these abnormal blood vessels and collect in the retina. The swelling caused due to this impairs vision.
Proliferative diabetic retinopathy (PDR), where new, but structurally unstable blood vessels grow on the surface of the retina. This in turn affects vision. One of the most serious consequences of proliferative retinopathy is tractional retinal detachment (separation of the layers of the retina) and vitreous hemorrhage.
Too much sugar in your blood can damage the tiny blood vessels that nourish the retina, sometimes blocking them completely. As more and more blood vessels become blocked, the blood supply to the retina gets cut, resulting in vision loss.
To compensate the lack of blood supply, the eye tries to grow new blood vessels. But, these new blood vessels don’t develop properly and are prone to leakage. Scar tissue may also form, which can exert a pull on the retina. Sometimes, this can cause tractional detachment of the retina.
Elevated blood sugar levels can also affect the eyes’ lenses. With high levels of sugar over long periods of time, the lenses can swell leading to cataract, providing another cause of blurred vision.
Worse cases of diabetic retinopathy can result in complications like:
If severe problems of dark spots, etc. are being experienced, treatment can start before sight is affected, thus, helping in preventing vision loss.
To diagnose diabetic retinopathy, a thorough examination of the retina is conducted. The ophthalmologist uses a lighted instrument called an ophthalmoscope. A dye may be used to reveal leaky blood vessels.
The treatment for diabetic retinopathy depends on the nature of the problem:
Call a doctor if you notice changes in your vision, particularly if they are sudden. Changes may include:
Hypertensive retinopathy is a complication that occurs in people who have high blood pressure. This high blood pressure often results in blood vessel abnormalities which may include thickening of the small arteries, blockages of retinal blood vessels and bleeding from them. Sudden and severe high blood pressure may also cause swelling of the optic nerve. All of this leads to hampering of vision. Lowering blood pressure can often stop ongoing damage to the retina. However, some existing damage can persist for which you must meet an experienced ophthalmologist.
There are often no particular symptoms that can be observed. Though some possible symptoms include:
Your primary aim should be to keep your blood pressure in check. Here are a few tips for it:
To diagnose hypertensive retinopathy, the ophthalmologist looks for pale or white areas of the retina using an ophthalmoscope (an instrument that projects light, to examine the back of your eyeball). During the examination, the ophthalmologist is looking for one of the following:
The only means of treating hypertensive retinopathy is to treat hypertension.
Call a doctor if you notice changes in your vision, particularly if they are sudden. Changes may include:
Copyright © 1987-2025 Ojas Eye Hospital All rights reserved | Privacy Policy
*Disclaimer: All information on www.lasikindia.com for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health care provider.